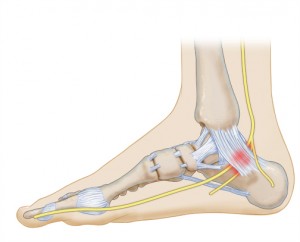
Tarsal tunnel syndrome, also known as posterior tibial neuralgia, is a squeezing or compression of the posterior tibial nerve that passes from the inside of the ankle into the foot. The condition is similar to carpal tunnel syndrome, which occurs in the wrist, as both disorders involve the compression of a nerve within an enclosed space. The symptoms of tarsal tunnel syndrome include numbness and pain, and may occur anywhere along the route of the tibial nerve.
What Is Tarsal Tunnel Syndrome?
Within the foot, there is a small canal running between the medial malleolus (the bump on the inside of the foot, which is part of the ankle bone) and the flexor retinaculum (the strip of ligaments reaching across the foot). This is known as the tarsal tunnel, and it contains the blood vessels, nerves and tendons that allow foot flexibility and movement. One of the nerves running through the tarsal tunnel is the tibial nerve; this nerve provides sensation to the bottom of the foot. Compression of the tibial nerve results in tarsal tunnel syndrome.
Causes of Tarsal Tunnel Syndrome
Many factors can lead to squeezing of the posterior tibial nerve, including:
- Injuries, such as ankle sprains, which may result in swelling and inflammation around the tarsal tunnel.
- Systemic diseases that cause swelling, such as arthritis and diabetes.
- Enlargement or abnormalities in any of the other structures running through the tarsal tunnel, for example varicose veins, swollen tendons, arthritic bone spurs, and ganglion cysts. The subsequent reduced space within the tunnel may compress the tibial nerve.
- Anatomical factors, including flat feet. The “fallen arch” observed in a flat foot may cause the heel to tilt outwards, which gives rise to strain and compression of the tibial nerve.
Symptoms of Tarsal Tunnel Syndrome
Tarsal tunnel syndrome is characterized by numbness, pain (often shooting pain), and a burning and tingling sensation that may feel like receiving an electric shock. Most patients experience these symptoms on the inside of the ankle or the bottom of the foot. The feeling may be confined to one spot, or spread to the toes, heel, arch of the foot or calf.
The disease is often exacerbated when the foot is overused, for example during exercise, prolonged standing, walking, or embarking on a new exercise regime. However, sometimes the symptoms can appear suddenly, with no apparent cause.
When to See a Doctor
Once symptoms become noticeable, it is imperative to see a doctor as soon as possible. If the condition is left untreated, the symptoms may progress and you may suffer irreversible nerve damage. In addition, tarsal tunnel syndrome is often confused with other conditions, so it is important to receive the correct diagnosis and treatment.
Diagnosis of Tarsal Tunnel Syndrome
The diagnosis of tarsal tunnel syndrome should be performed by a specialist neurologist. After the doctor has taken a thorough medical history and conducted a physical examination, electrical testing (either electromyography or a nerve conduction study) and imaging, through an MRI, an X-ray or a CT scan, can confirm the diagnosis. Disease severity also needs to be assessed to determine the type of treatment; in severe cases of tarsal tunnel syndrome, surgery may be required.
Tarsal Tunnel Syndrome Treatment
1. Non-Surgical Treatment
Various types of non-surgical tarsal tunnel treatment are available to treat tarsal tunnel syndrome, including:
- Rest: The symptoms of tarsal tunnel syndrome may be reduced by avoiding any physical activity that worsens the pain. Resting your affected foot can encourage healing and prevent further injury.
- Apply an ice pack: An ice pack can help in reducing the compression of the strain and compression of the tibial nerve. Put a thin towel on the affected area, and then apply an ice pack on the towel. Apply it for 20 minutes. After that, wait at least 40 minutes before applying again.
- Take medications: If the symptoms are unbearable, you can take nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, which help reduce the pain and inflammation of your foot.
- Wear a cast: In order to enable the tibial nerve and surrounding tissues to heal, sometimes it is necessary to wear a cast to restrict the movements of your foot.
- Use physical therapies: Your doctor may recommend you some physical therapies which include stretching exercises, ultrasound therapy, and others to reduce the symptoms of tarsal tunnel syndrome.
- Stretching exercises: If the gastrocnemius and soleus muscles, which comprise the calf muscle group, become tight, this can increase over-pronation of the foot. Therefore it is essential to properly stretch the calves. Remember that exercise should never be painful.
First, you’ll need to examine your calf muscle flexibility. The suppleness of the gastrocnemius muscle can be assessed by lying down on your back on a couch with your feet hanging off the end. Your therapist should be able to gently push each of your feet to a 90 degree angle, and you will feel a slight resistance, although the movement shouldn’t be forced.
To stretch the soleus muscle, which is lower down the leg than the gastrocnemius, start by standing facing a wall. Place the leg you want to stretch behind the other leg and bend both knees. Make sure that your heels are pressed into the ground, lean forward into the wall until you notice a stretch. If you can’t feel this stretch, try raising the front of the foot by placing an object under the toes, or place your foot up against the wall, pushing the knee forwards.
- Try injection therapies: You doctor may also perform injection therapies. Injections of a local anesthetic on the affected area can provide pain relief and injections of corticosteroid may also help in treating the inflammation of the affected tissue.
- Use orthotic devices and supportive shoes: To relieve the pain and inflammation of your foot, you can use shoe inserts to limit excessive motion of your foot which can cause compression of the tibial nerve and maintain the arch. You can also wear supportive shoes to ease the symptoms.
2. Surgery
If symptoms have not improved following conventional therapies, surgical decompression, via sectioning of the flexor retinaculum, needs to be considered. To prevent nerve fibrosis developing, the decompression should be carried out as soon as possible. In terms of improving symptoms, tarsal tunnel relief has produced impressive results.
Prognosis
After surgery, 85-90% patients find that the symptoms of tarsal tunnel syndrome are relieved or improved.
Watch the following video to learn more information about tarsal tunnel syndrome:
